Respirator Use and Practices in Primary Metal Operations
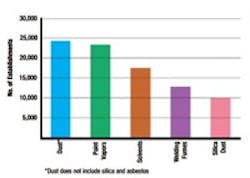
The most common substances for which manufacturers assign respirators to their workers.
In 2001 the U.S. Labor Dept.'s Bureau of Labor Statistics (BLS) and the National Institute for Occupational Safety and Health (NIOSH) conducted the Survey of Respirator Use and Practices among 40,000 randomly selected U.S. establishments. 1 The topics surveyed and data collected included the types of respiratory protection used by workers, the types of respirator fit tests performed, and the presence of substances that prompted the decision to use respiratory protection.The findings of the survey raised questions about respirator usage, and how these practices compare with Occupational Safety and Health Administration (OSHA) regulations2 and NIOSH recommendations.3 This report focuses on information from the survey for establishments in the Primary Metal Industries, i.e., steel works; blast furnaces; rolling and finishing mills; iron and steel foundries; and primary nonferrous smelters and refineries (Standard Industrial Classification 33).4
Findings and discussion — Approximately 28%, or an estimated 2,043 Primary Metal Industries establishments, had their workers using respirators. This percentage was higher than the percentage of establishments with respirator use in its parent industry, Manufacturing, and All Private Industry (12.8% and 4.5%, respectively). Among the types of respirators in use, air-supplied respirators were used in 7.9% of Primary Metal Industries establishments.1 Also, employees in Primary Metal Industries used respirators in greater proportions than employees in All Private Industry as a whole (14.0% vs. 3.1%).
Typical Primary Metal Industries operations (e.g., pouring, drossing, moldmaking, abrasive blasting, chipping, grinding, and welding) can result in exposures to airborne contaminants and agents (metal fumes, silica dust, formaldehyde, and isocyanates) that are associated with various respiratory conditions. For example, silica-dust exposure can cause silicosis5,6 and isocyanate exposure can cause asthma.6,7,8,9
While the survey did not allow determination of particular substances that prompted respirator use within Primary Metal Industries, it did so for the parent industry, Manufacturing. Dust, paint vapors, solvents, welding fumes, and silica dust were the substances for which respirators were most frequently used (see graph). Less frequently reported substances were vapors (except paint vapors), toluene, acid gas, carbon monoxide, and lead.
Of the respirator-using Primary Metal Industries establishments, nearly half (48%), or an estimated 900 establishments, had three or more indicators of a potentially inadequate respiratory protection program, as measured against OSHA's respirator program requirements (see below.) This indicates a need for improvements in respiratory protection programs in these establishments.
The survey findings are subject to some limitations. Public sector, self-employed, and agricultural establishments with less than 11 workers were not included in the survey. Although the instructions stated that the person most familiar with respiratory protection should complete the questionnaire, this may not have happened in all instances. In spite of the cognitive and field testing of the survey at small, medium, and large establishments prior to its mailing, even knowledgeable persons may have misinterpreted the written questions.
OSHA's respirator program requirements — Each of the indicators listed here (based on OSHA requirements2) is an important part of an effective respirator program. If the answer to any of these questions is "no," it may indicate that an operation's overall quality of respiratory protection is inadequate, and may need improvement:
• Does it include a trained respirator program administrator?
• Has management adopted a written respirator program that determines how respirators are used?
• Does it include written procedures for maintaining respirators?
• Are wearers of tight-fitting respirators fit-tested?
• Are employees assessed for medical fitness to wear respirators?
• Does the program provide training regarding the need, use, limitations, and capabilities of respirators?
• Do written procedures include a periodical evaluation of the effectiveness of respirators used at the establishment?
• Are airline respirator couplings incompatible with other gas systems at the establishment?
• Does the program require manufacturer's instructions or NIOSH certification labels to adjust the airflow for airline respirators?
• Is there a written change-out schedule for air-purifying gas/vapor filters?
• Are dust masks used (filtering-facepiece respirators) to protect only against dusts, but not gases or vapors?
These findings and conclusions are those of the authors and do not necessarily represent the views of the National Institute for Occupational Safety and Health. For more information, contact Brent Doney at 304-285-6357, or [email protected]
Needed: Improved respiratory protection programs —The number of indicators of potentially inadequate respiratory protection programs in Primary Metal Industries demonstrates a need for improvement. It is the obligation of each establishment to evaluate its own respiratory protection program with respect to the OSHA requirements2, and NIOSH recommendations and make appropriate changes.
Employers who suspect their respiratory protection program is in need of improvement should consider contacting OSHA for free, confidential consultation available to small businesses in every state. OSHA also has a "Small Entity Compliance Guide for the Respiratory Protection Standard," available at www. osha.gov. Another resource is the American Industrial Hygiene Association's list of consultants, at www.aiha.org.
References
- Bureau of Labor Statistics/National Institute for Occupational Safety and Health [2003]. Respirator Usage in Private Sector Firms, 2001. Washington, DC.
- Code of Federal Regulations [1998]. Occupational Safety and Health Administration, Respiratory Protection Standard, 29 CFR 1910.134.
- NIOSH [2005]. NIOSH Respirator Selection Logic 2004. Cincinnati, OH: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, DHHS (NIOSH) Publication No. 2005 100.
- Office of Management and Budget [1987]. Standard Industrial Classification Manual. Washington, DC: U.S. Government Printing Office.
- 5. CDC [2005]. Silicosis Mortality, Prevention, and Control – United States, 1968– 2002. MMWR Morb Mortal Wkly Rep 54:401–5.
- NIOSH [2003]. Work-related Lung Disease Surveillance Report 2002. Cincinnati, OH: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, DHHS (NIOSH) Publication No. 2003 111.
- CDC [2002]. Asthma Prevalence and Control Characteristics by Race/Ethnicity – United States, 2002. MMWR Morb Mortal Wkly Rep 53:145–8.
- NIOSH [2006]. NIOSH Alert, Preventing Asthma and Death from MDI Exposure During Spray-on Truck Bed Liner and Related Applications. Cincinnati, OH: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, DHHS (NIOSH) Publication No. 2006 149.
- Westberg H, Lofsted H, Selden A, et al. [2005]. Exposure to Low Molecular Weight Isocyanates and Formaldehyde in Foundries Using Hot Box Core Binders. Ann Occup Hyg 49:719–25.
Brent Doney is a certified industrial hygienist; Mark Greskevitch is an industrial hygienist; and Girija Syamlal and Ki Moon Bang are epidemiologists. All of them are affiliated with the National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies (www.cdc.gov/niosh/topics/surveillance/ORDS/), in Morgantown, WV.
Dennis Groce is a certified industrial hygienist with EG&G Technical Services Inc. (www.urscorp.com/EGG_Division), Pittsburgh, provides management and technical services to the U.S. Depts. of Defense and Homeland Security and other federal agencies.